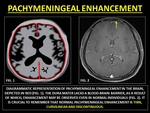
PACHYMENINGEAL ENHANCEMENT (PE)
PE is best appreciated on a contrast-enhanced MRI (CE-MRI). (14,
15) The dura is devoid of the BBB and is permeable to contrast.
PE is seen along the cerebral convexities or its reflections.(14) Thin,
discontinuous enhancement may be normal.(15)
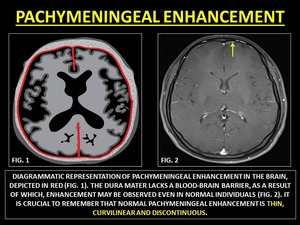
Fig. 6: REPRESENTATIVE IMAGES OF PACHYMENINGEAL ENHANCEMENT
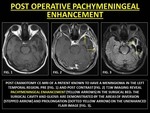
Post-operative PE is does not necessarily indicate recurrence.
Surgically induced PE is attributed to an inflammatory response or chemical arachnoiditis secondary intra-operative bleeding.(16) A follow-up to ensure interval stability or regression, is recommended.
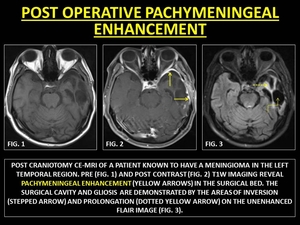
Fig. 7: POST OPERATIVE PACHYMENINGEAL ENHANCEMENT
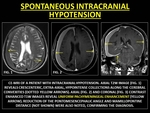
Intracranial hypotension (IH) may be due to traumatic injury or may be idiopathic.
(17) Diffuse PE is a classical finding,
occuring due to vasocongestion and interstitial edema in the dura secondary to fluid shifts which increase the volume of subarachnoid capacitance veins as the cerebrospinal fluid pressure drops. These fluid shifts lead to subdural collections. PE associated with intracranial hypotension is diffuse but never involves the leptomeninges. (17)
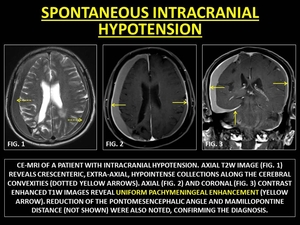
Fig. 8: SPONTANEOUS INTRACRANIAL HYPOTENSION
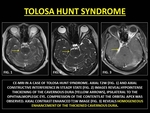
Tolosa Hunt syndrome is a rare granulomatous dural inflammation characterized by episodes of ophthalmoplegia.
(18) It affects the dura of the cavernous sinus and/or superior orbital fissure (SOF) causing pressure effects on its neurovascular contents (19) CE-MRI findings include enhancing thickening of the cavernous dura with extension into the orbital apex through the SOF with variable degrees of cranial nerve compression.
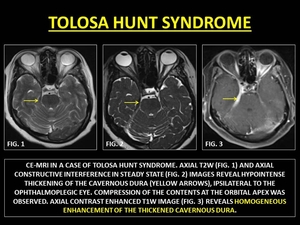
Fig. 9: TOLOSA HUNT SYNDROME
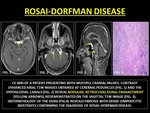
Rosai-Dorfman disease (RDD) is an uncommon condition characterized by cervical lymphadenopathy.
The intracranial manifestation of RDD is dural-based masses along the parasellar,
cavernous sinus,
retroclival,
cerebellopontine angle and parafalcine regions.
Though imaging features mimic meningiomas,
profound T2W hypointensity in RDD is due to inflammatory free radicals.
Angiography also distinguishes meningiomas (hypervascular) from RDD (avascular).
(20)
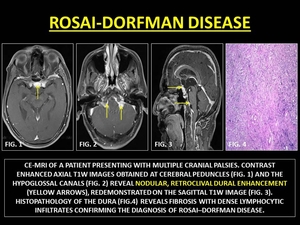
Fig. 10: ROSAI-DORFMAN DISEASE
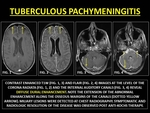
Tuberculous Pachymeningitis (TBP) is distinct from the dural inflammation near an intraparenchymal tuberculoma and is secondary to hematogenous dissemination.
Imaging features of TBP are non-specific,
ranging from focal dural thickening to diffuse PE.
TBP is essentially a diagnosis of exclusion where clinicopathological workup helps the radiologist.
(21)
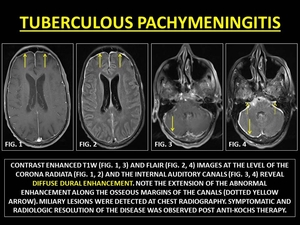
Fig. 11: TUBERCULOUS PACHYMENINGITIS
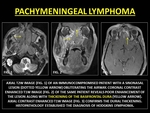
Secondary lymphoma (SCNSL) is almost invariably metastatic.
SCNSL is extremely rare and is biologically distinct from other PCNSL,
which tend to be intraparenchymal.
Pachymeningeal SCNSLs are seen as diffuse enhancing masses along the convexities/falx/tentorium/sellar/parasellar regions.
(22-24)
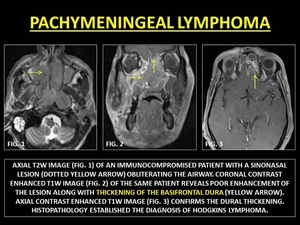
Fig. 12: PACHYMENINGEAL LYMPHOMA
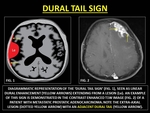
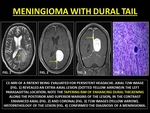
Dural Tail is the linear,
enhancing,
tapering rim of pachymeningeal thickening (PT) adjacent to a lesion.
It may be smooth or nodular and may be 0.5 to 3.0 cm long.
It occurs due to tumor invasion or reactive PT.
Dural tails are associated with meningiomas,
other extra-axial lesions (haemangiopericytomas,
metastasis) and some peripherally located intra-axial lesions (neuromas,
chloromas,
metastasis,
lymphoma,
gliomas,
granulomatous disorders,
and Erdheim-Chester disease). (25-29)
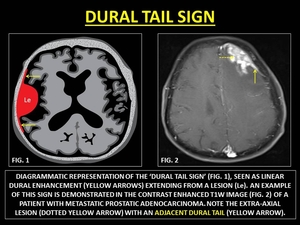
Fig. 13: REPRESENTATIVE IMAGES OF 'DURAL TAIL SIGN'
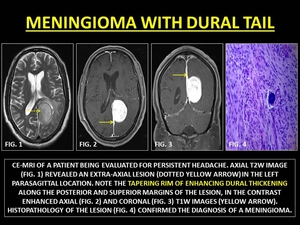
Fig. 14: MENINGIOMA WITH DURAL TAIL
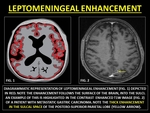
LEPTOMENINGEAL ENHANCEMENT
Leptomeningeal enhancement (LE) refers to enhancement of the pia-arachnoid. LE extends into the sulci and cisterns of the brain.
(14)
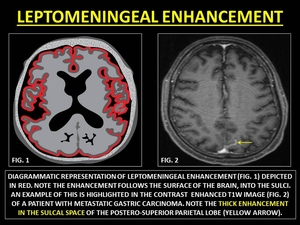
Fig. 15: REPRESENTATIVE IMAGES OF LEPTOMENINGEAL ENHANCEMENT
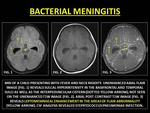
Bacterial leptomeningitis is a common CNS infection. Glycoproteins released by bacteria cause BBB breakdown.
(14) At CE-MRI,
bacterial leptomeningitis is typically thin and linear along the sulcal spaces and basal cisterns.
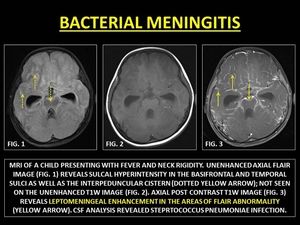
Fig. 16: BACTERIAL MENINGITIS
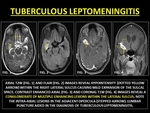
Tuberculous Leptomeningitis occurs as a result of hematogenous dissemination of tubercular bacteria.
LE in such cases is characterized by a thick enhancement in the region of basal cisterns and the Sylvian fissure.
Sulci over the convexities are less dominantly affected.
(30)
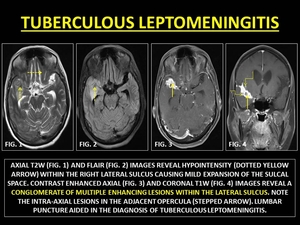
Fig. 17: TUBERCULOUS LEPTOMENINGITIS
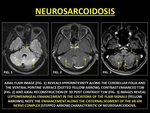
Sarcoidosis typically involves lungs and lymph nodes.
It rarely involves the CNS.
Leptomeningeal involvement is the most common manifestation of neurosarcoidosis.
CE-MRI in neurosarcoidosis reveals thick,
sometimes nodular LE,
with a basilar predilection. Cranial nerves (CNs) may also be involved along with leptomeningeal disease. (31)
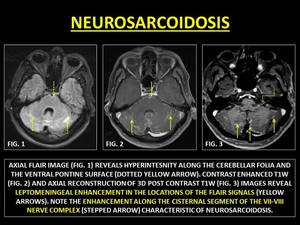
Fig. 18: NEUROSARCOIDOSIS
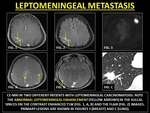
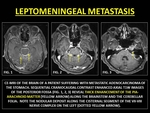
Leptomeningeal carcinomatosis (LCM) is the metastatic leptomeningeal infiltration by malignant cells originating from an extrameningeal neoplasm that may be extraneural or intraneural. Common extraneural sites include breast,
lung,
skin,
gastrointestinal tract,
lymphoma and the head-neck,
while intraneural sites include medulloblastomas,
ependymomas,
glioblastomas,
and oligodendrogliomas.
LCM produces thick,
enhancement but may also be surprisingly thin and linear. (14,
32)
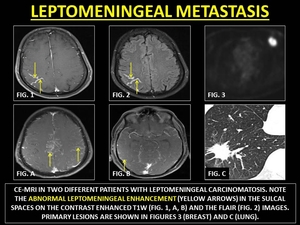
Fig. 19: LEPTOMENINGEAL METASTASIS
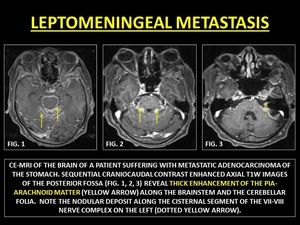
Fig. 20: LEPTOMENINGEAL METASTASIS
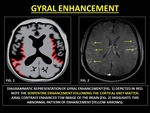
GYRAL ENHANCEMENT
Gyral enhancement (GYE) refers to serpentine ‘gyriform’ enhancement along the grey matter.
A host of factors may lead to such abnormal enhancement ranging from infective to vascular etiologies.
(14)
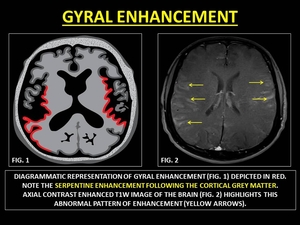
Fig. 21: REPRESENTATIVE IMAGES OF GYRAL ENHANCEMENT
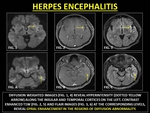
Herpes encephalitis (HE) occurs due to infection by the herpes simplex virus 1 (HSV1).
CNS manifestations occur as a result of reactivation of dormant HSV1 infection.
Initially,
it initially gains CNS entry via the nasopharynx with retrograde dissemination along trigeminal nerve into the trigeminal ganglion,
where it is harbored indefinitely.
Reactivation may be spontaneous or induced by stressors.
MRI reveals restricted diffusion in the limbic cortices in early stages.
GYE is seen in the later stages and occurs due to the breakdown of the BBB.
(33)
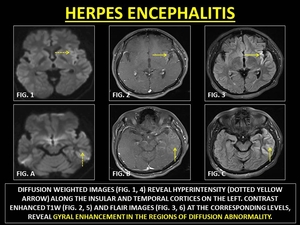
Fig. 22: HERPES ENCEPHALITIS
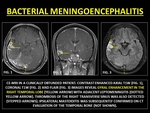
Pyogenic Meningoencephalitis (PME) is the result of bacterial spread of from extracranial foci or following trauma.
Myriads of bacteria can cause can cause PME,
commonly including Streptococcal and Staphylococcal species.
Cerebritis in these infections leads to hypercellularity,
brain ischemia,
and/or cytotoxic edema; which contribute to the breach of the BBB.
Early cerebritis often shows little or no GYE on CE-MRI,
subsequently organizing into an abscess.
(34)
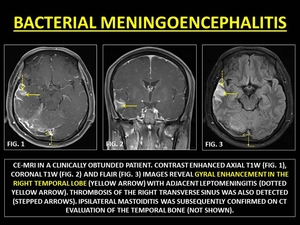
Fig. 23: BACTERIAL MENINGOENCEPHALITIS
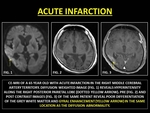
Acute Cerebral Infarction (ACI) leads to a GYE within the 1st week of its occurrence due to breakdown of the BBB. It must not be confused with Hyperintense Acute Reperfusion Marker (HARM),
which refers to the enhancement of the subarachnoid space.
Occasionally GYE may be delayed,
either due to the time needed for neoangiogenesis or due to the time taken for the diminution of the vasogenic edema.
(35)
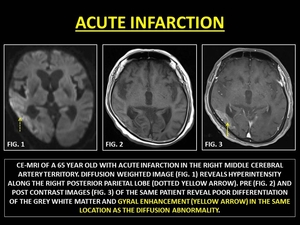
Fig. 24: ACUTE INFARCTION
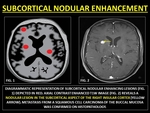
SUBCORTICAL NODULES
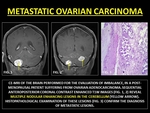
Metastasis to the brain is the most common site of intracranial neoplastic dissemination (80%).
Hematogeneous metastases have a predilection for arterial border zones and the cortico-medullary junction due to the tapering of vessels at these junctions.
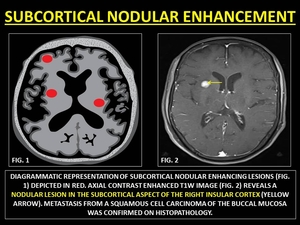
Fig. 25: REPRESENTATIVE IMAGES OF SUBCORTICAL NODULAR ENHANCEMENT
Metastatic disease arising from primary pelvic malignancies is carried into the retroclival venous plexus by the Batson venous plexus.
Therefore,
a preference of the infratentorial compartment is seen in metastatic lesions from pelvic primaries.
(14)
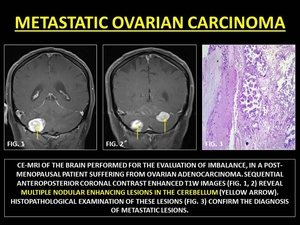
Fig. 26: METASTATIC OVARIAN CARCINOMA
PERIPHERALLY ENHANCING LESIONS
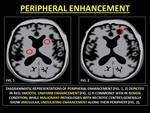
Peripherally enhancing lesions or ring-enhancing lesions (RELs) frequently encountered in neuroradiology.
As a general rule benign lesions are smooth uniform RELs,
while malignant lesions are thick,
irregular RELs.
(36,
37)
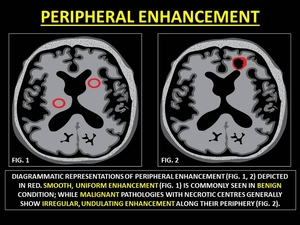
Fig. 27: REPRESENTATIVE IMAGES OF PERIPHERAL ENHANCEMENT

Fig. 28: DIFFERENTIAL DIAGNOSIS OF PERIPHERALLY ENHANCING LESIONS
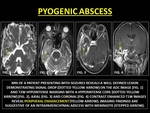
Pyogenic Abscesses evolve through the phases of cerebritis.
In the early capsular stage,
abscesses are well-delineated with thin, smooth peripheral enhancement.
In the late phase a T2W hyperintense core with an irrregular enhancing rim is observed on CE-MRI is observed. (34)
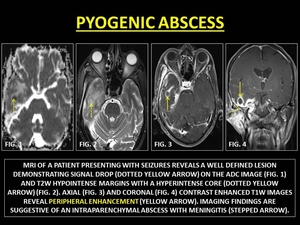
Fig. 29: PYOGENIC ABSCESS
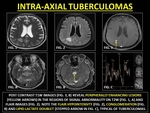
Tuberculoma (TB granuloma) as a focal parenchymal granulomatous infection with central caseating necrosis varying,
in size from miliary nodules to lesions as large as 4-6 cm.
Lesions appear hypointense on T2WI due to the caseous necrosis with ring-enhancement.
(34)
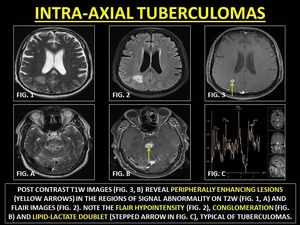
Fig. 30: INTRA-AXIAL TUBERCULOMAS
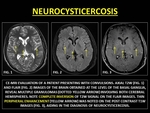
Neurocysticercosis is a CNS infection by the secondary larval form of the Taenia solium.
The phases of its evolution include vesicular,
colloidal vesicular,
granular nodular and nodular calcified.
Ring enhancement is seen in the colloidal vesicular stage (in which the larvum is killed by the host response).
(34)
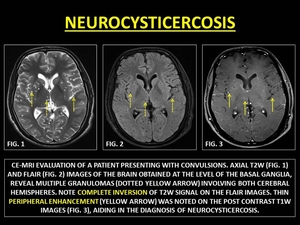
Fig. 31: NEUROCYSTICERCOSIS
Tuberculoma,
a major differential,
shows absence of central inversion on FLAIR imaging,
restricted diffusion and a lipid peak on spectroscopy.
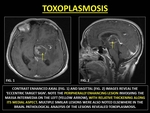
Neurotoxoplasmosis is an opportunistic infection common in immunocompromised patients.
Imaging reveals an ‘eccentric target sign’, described as a small eccentric nodule along the wall of the lesion.
The nodule is produced by thickened vessels traversing the sulcus while the peripheral rim of enhancement reflects dense histiocytic response.(38)
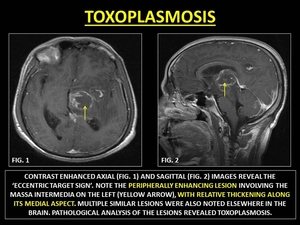
Fig. 32: TOXOPLASMOSIS
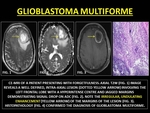
Glioblastoma Multiforme (GBM) is a malignant primary CNS lesion,
usually microscopically necrotic and macroscopically cavitating with prominent peripheral neovascularity with abnormal BBB.
The enhancing rim,
contains the greatest concentration of neovascularity and is often thick and on the cortical or outer surface and thinner on the white-matter margin. (14)
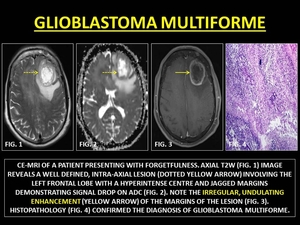
Fig. 33: GLIOBLASTOMA MULTIFORME
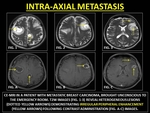
Metastatic lesions are seen in the subcortical aspect of the brain parenchyma.
Signal heterogeneity is common in metastasis with irregular peripheral enhancement due to the peripheral neoangiogenesis and disruption of the BBB.
(39)
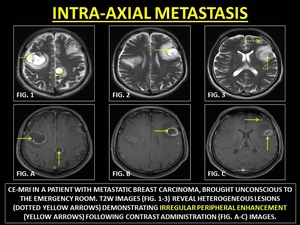
Fig. 34: INTRA-AXIAL METASTASIS
SPECIAL CONSIDERATIONS
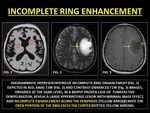
Incomplete ring enhancement (IRE) is encountered in demyelination,
typically multiple sclerosis (MS).
Plaques of MS enhance during the “active phase,” due to inflammation,
often limited to the venous side.
Enhancement is not due to neovascularity,
angiogenesis,
or necrosis.
CE-MRI may show IRE with the incomplete portion directed towards the cortex.
The enhanced portion represents active inflammation,
while the unenhanced portion represents a chronic inflammatory process.
(14,
40)
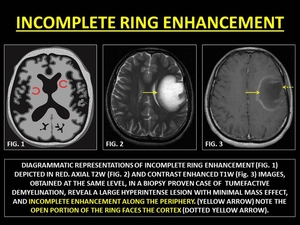
Fig. 35: INCOMPLETE RING ENHANCEMENT
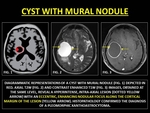
Cyst with Mural Nodule Tumor (CMNTs) is a subtype of intra-axial enhancement caused by fluid-secreting low-grade primary neoplasms.
The term cyst is a misnomer,
as true cysts are lined by an epithelium and would not enhance.
In CMNTs,
part of the rim may not enhance,
due to tissue compression or gliosis.
(14,
41)
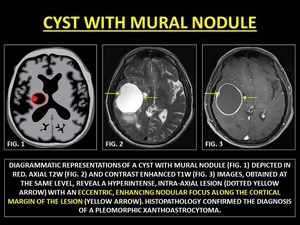
Fig. 36: CYST WITH MURAL NODULE
PERIVENTRICULAR LESIONS
Of the all the periventricular lesions,
CNS lymphomas,
primary glial tumors and infections are the common causes of enhancement in this location.
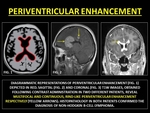
Primary CNS lymphoma [PCNSL] are commonly of non-Hodgkin's B-cell type.
These occur,
in immunocompetent as well as compromised individuals,
as a solitary homogeneously enhancing periventricular lesion located in supratentorial compartment.
Classically,
they present in a ‘butterfly' pattern across the corpus callosum.
(42)
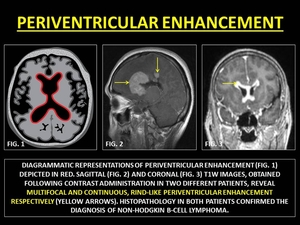
Fig. 37: PERIVENTRICULAR ENHANCEMENT
References: CORONAL T1W CONTRAST ENHANCED IMAGE (FIG. 3) CONTRIBUTED BY DR. PRASHANT MUDGAL.
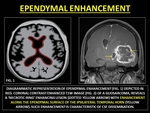
EPENDYMAL ENHANCEMENT
The ependyma is a thin membrane of glial cells lining the ventricles of the brain and the central canal of the spinal cord.
Enhancement of the ependyma may be smooth or nodular and often missed in the background of a intraparenchymal lesion.
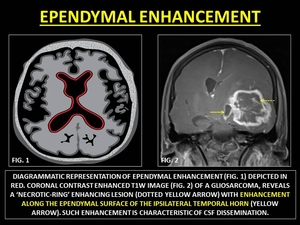
Fig. 38: REPRESENTATIVE IMAGES OF EPENDYMAL ENHANCEMENT
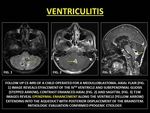
Pyogenic Ventriculitis is the bacterial infection of the ventricular system and is an important source of persistent infection in treated cases of meningitis.
Pathogens are usually gram-negative bacteria. MRI may reveal,
dependent layering of exudates in the ventricles (with restricted diffusion),
hydrocephalus and/or periventricular ooze. CE-MRI reveals thin ependymal contrast enhancement.
Astrocytic proliferation,
ependymal fibrosis and subependymal gliosis may be seen in the chronic phases of ventriculitis.(43)
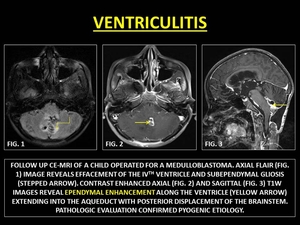
Fig. 39: VENTRICULITIS
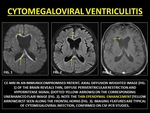
Cytomegaloviral (CMV) Ventriculitis usually occurs when in the immunocpromised when CD4+ counts fall below 50 cells/μ. A ten-fold higher incidence of ventriculitis is seen in patients who develop CMV retinitis.
MRI in CMV infections may produce a suggestive pattern of ependymitis,
seen as subependymal and periventricular T2W hyperintensity and restricted diffusion.
CE-MRI reveals thin ependymal enhancement.
(44)
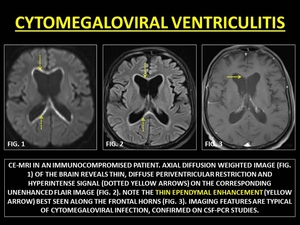
Fig. 40: CYTOMEGALOVIRAL VENTRICULITIS
Dissemination of High Grade Gliomas and Metastasis to the ventricles are not uncommon.
The ependyma is the important routes of spread of malignant brain lesions,
particularly gliomas.
Gliomas occur in the supratentorial compartment.
Spread along the ependyma seeds malignant cells in the infratentorial compartment as well as along the spinal cord.
The interval between the intracerebral GBM and these metastasis is 12-14 months and the mean survival time,
never exceeds 6 months.
(45)
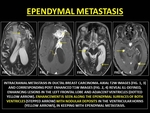
The atria of the lateral ventricles are common sites of metastatic spread diseases.
Common primaries sites include kidneys, lung,
skin,
stomach,
colon,
breast and lymphoma.
CE-MRI reveals nodular or smooth enhancement along the ependyma. (46)
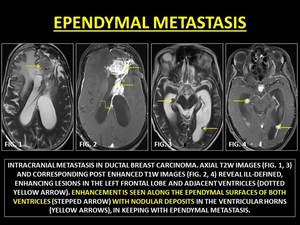
Fig. 41: EPENDYMAL METASTASIS